- Pancreaticojejunostomy guided by the theory of mucosal priority healing
- Global and Chinese disease burden of alcoholic pancreatitis and its causal association with alcohol consumption
- Injury severity-dependent differences in pancreatic regeneration and repair in cerulein-induced acute pancreatitis
- Laparoscopic spleen-preserving distal pancreatectomy combined with autologous islet transplantation for intraductal papillary mucinous neoplasms: a case report and literature review
- Application of Y-shaped reconstruction using allogeneic common iliac vein and its branches in pancreatic cancer with long-segment portal vein-superior mesenteric vein involvement
- Comparison of single-incision plus one-port versus conventional muti-port laparoscopic common bile duct exploration
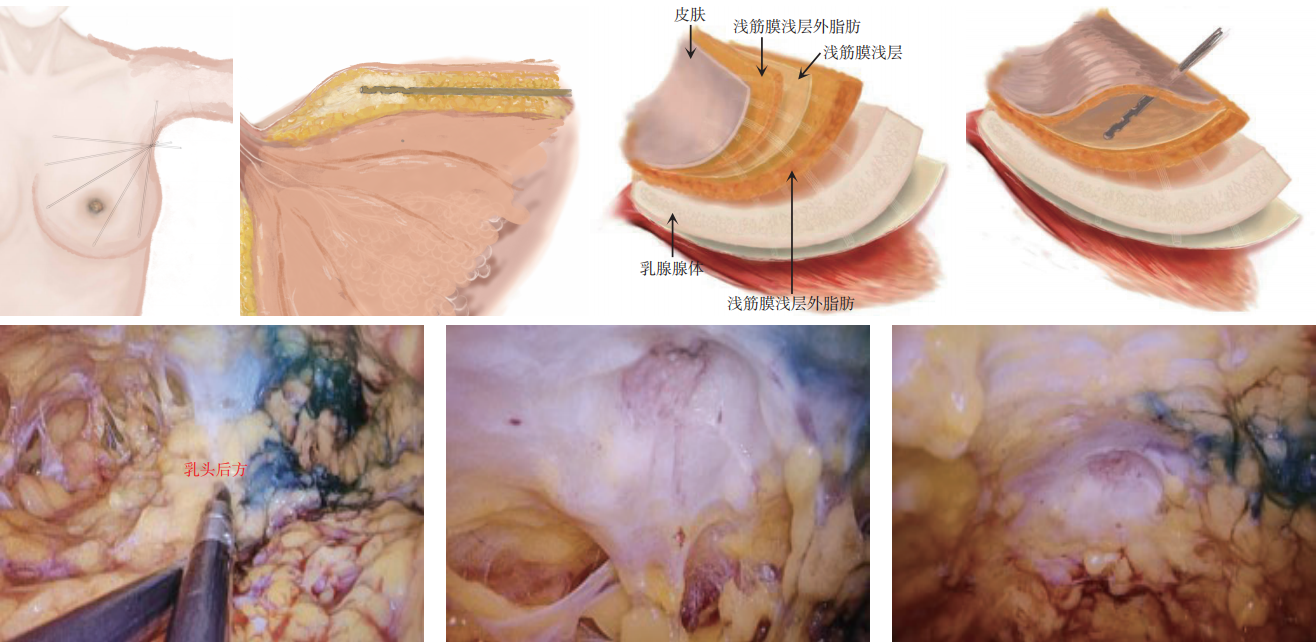
- Technical key points of endoscopic electro-scissors-assisted subcutaneous glandular excision of the breast via a single-port axillary approach
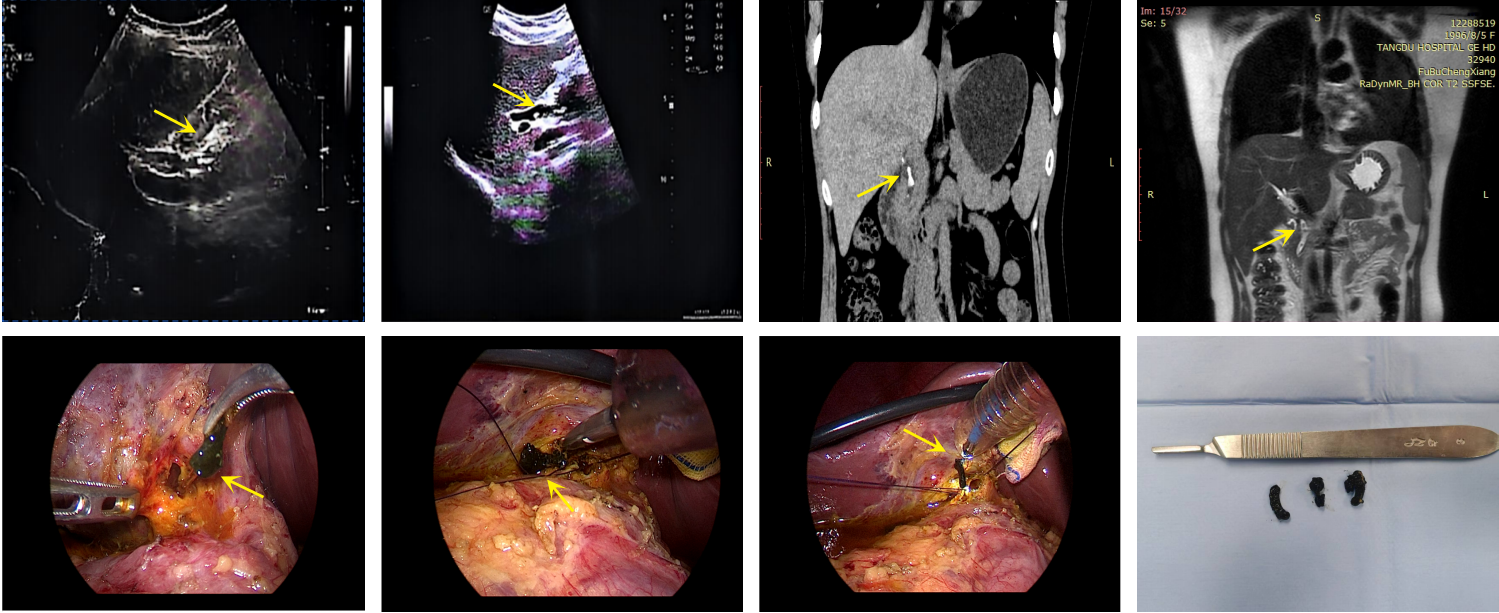
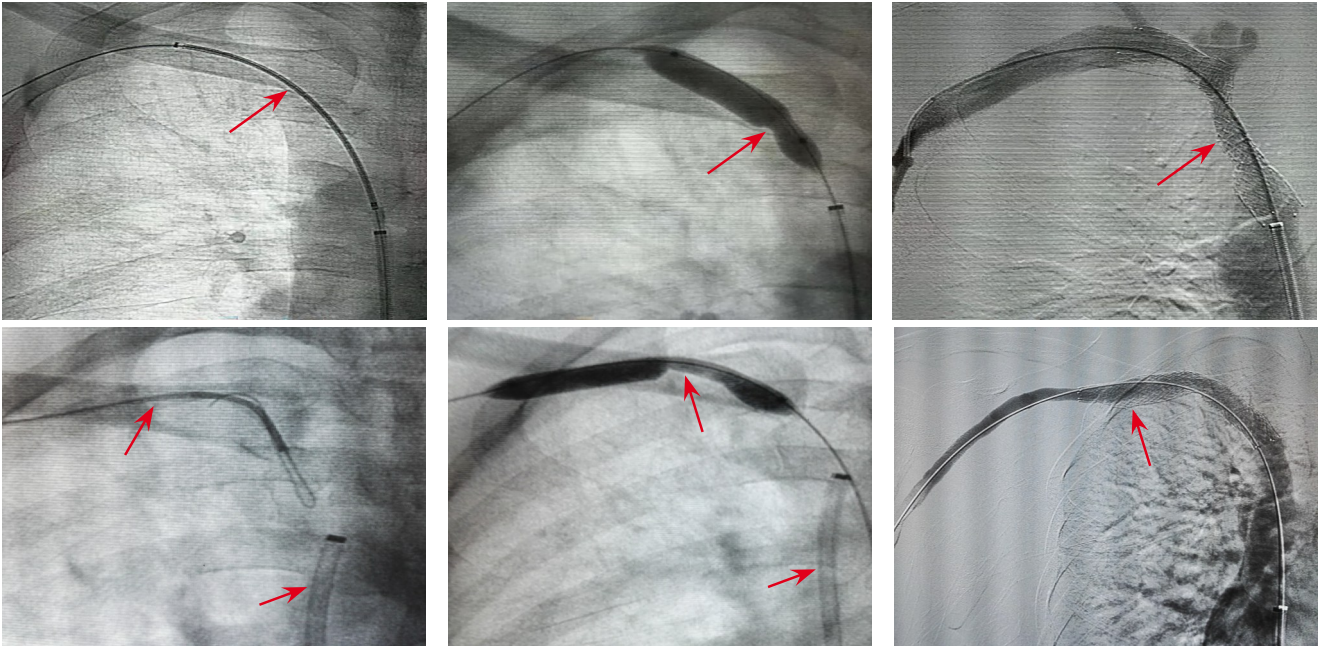
- Diagnosis and treatment of Hem-o-lok clip migration into the common bile duct after laparoscopic cholecystectomy: a case report and literature review
- Auxiliary liver transplantation using discarded liver: innovative clinical applications and future perspectives
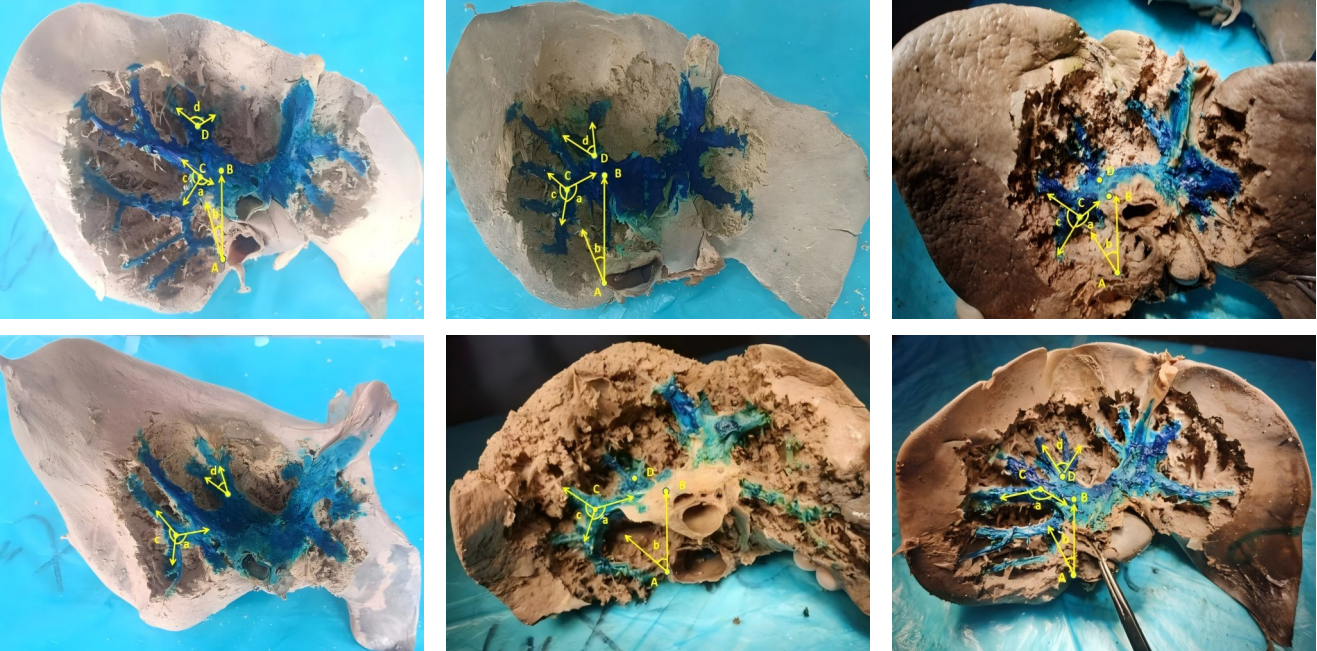
- Applied anatomy of segmental Glissonian pedicles at the hepatic hilum guided by the Laennec's membrane concept and its value in laparoscopic surgery
- Application of augmented reality navigation combined with indocyanine green fluorescence imaging in laparoscopic resection of central hepatic tumors
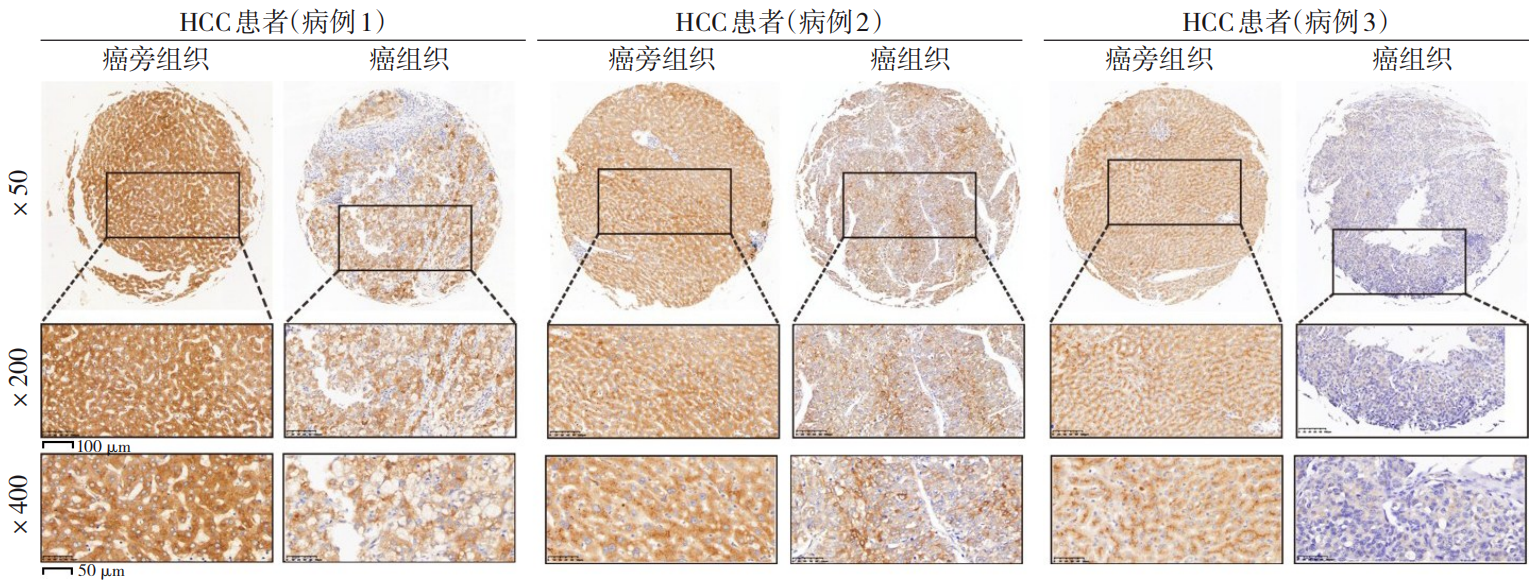
- Expression characteristics of FGL1 in peritumoral tissues of hepatocellular carcinoma and its association with prognosis
- Expert consensus on fibrin sealant aneurysm sac filling during endovascular abdominal aortic aneurysmal repair
- Comparison of venous access strategies for endovascular management of central venous stenosis or occlusion in hemodialysis patients
- Current Issue
- Published Ahead-of-Print
- Virtual Issues
- Previous Issues
-
Pancreatic Surgery Working Group, General Surgery Professional Committee, Hunan Medical Association
2026,35(3):403-419, DOI: 10.7659/j.issn.1005-6947.260004
Abstract:
Acute pancreatitis (AP) is a common acute abdominal condition with significant regional variations in incidence worldwide. Hunan province, characterized by a high prevalence of biliary diseases, has a relatively high and steadily increasing incidence of AP. Notably, substantial disparities in diagnostic and therapeutic capabilities exist across different regions and healthcare levels, which may adversely affect patient outcomes. To standardize the management of AP and improve the overall quality of care, the Pancreatic Surgery Working Group of the General Surgery Professional Committee of the Hunan Medical Association developed this standardized protocol based on expert consensus, incorporating current domestic and international guidelines as well as recent advances. The protocol systematically addresses diagnostic criteria, etiological evaluation, clinical manifestations, laboratory and imaging assessments, severity stratification, disease staging, complication management, and follow-up strategies. Implementation of this protocol is expected to enhance early recognition and diagnostic accuracy, optimize stratified treatment, and reduce complications and mortality, particularly improving outcomes in patients with severe AP.
-
CAI Zhenghua, MAO Liang, QIU Yudong
2026,35(3):420-428, DOI: 10.7659/j.issn.1005-6947.260097
Abstract:
Artificial intelligence (AI) is rapidly being integrated into the entire workflow of pancreatic surgery, driving the transition toward precision and intelligent surgery in this highly complex field. In the preoperative setting, deep learning-based image segmentation and three-dimensional reconstruction enable precise delineation of pancreatic tumors and surrounding vasculature, facilitating surgical planning and resectability assessment. Intraoperatively, technologies such as augmented reality navigation and real-time tissue recognition assist in anatomical localization and risk identification, thereby improving surgical accuracy and safety. Postoperatively, AI-driven models integrating multi-source clinical data allow early prediction of complications and support individualized management. However, several challenges remain, including data heterogeneity, limited model interpretability, and the lack of standardized pathways for clinical translation. This review systematically summarizes the current applications of AI in preoperative planning, intraoperative navigation and decision-making, and postoperative complication management in pancreatic surgery, and further discusses existing challenges and future directions. Future efforts should focus on the development of high-quality multicenter standardized databases, multimodal and interpretable AI models, and closed-loop intelligent surgical systems integrating perception, decision-making, and execution, to facilitate the standardized implementation and clinical translation of AI technologies.
-
WU Shixing, LI Jiangang, GENG Cheng, WANG Cheng, ZHANG Bolin, ATIGU·Abuduwaili, XU Xinjian, TANG Zhaohui
2026,35(3):429-435, DOI: 10.7659/j.issn.1005-6947.250567
Abstract:
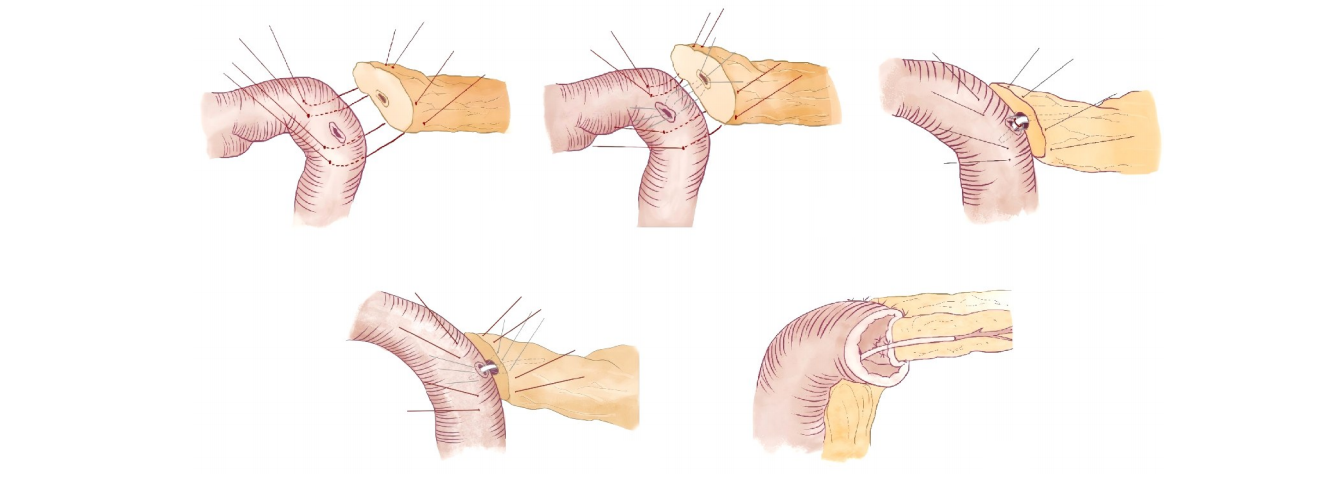
Pancreaticojejunostomy is a critical step in pancreatoduodenectomy, and its quality directly affects the incidence of postoperative complications, including pancreatic fistula and hemorrhage. Despite continuous technical improvements, the risk of severe complications remains substantial. Based on pathological observations and histological analyses, and considering the migration characteristics of intestinal mucosa, we propose the concept of "mucosal priority healing". This concept emphasizes shortening the migration distance of intestinal mucosa and reducing the number of anastomotic sutures to facilitate rapid apposition and healing between the jejunal mucosa and the pancreatic duct epithelium. Pancreaticojejunostomy guided by this concept optimizes the healing mechanism of the anastomosis, ensures adequate pancreatic drainage, and may reduce the risk of severe complications such as postoperative hemorrhage, reoperation, and mortality. This article systematically reviews the theoretical basis, technical features, and clinical outcomes of this approach, and discusses future research directions in the context of current evidence, aiming to provide insights into the standardization and precision of pancreaticojejunostomy.
-
ZHUO Junzhe, LUO Qilan, WANG Min
2026,35(3):436-445, DOI: 10.7659/j.issn.1005-6947.260066
Abstract:
Minimally invasive pancreaticoduodenectomy (MIPD) is transitioning from a stage of technical feasibility toward a phase focused on achieving oncologic radicality while maintaining safety. Current evidence suggests that, in high-volume centers with experienced surgical teams, the perioperative safety of MIPD is comparable to that of open pancreaticoduodenectomy. However, its safety profile is influenced not only by the surgical approach, but also by institutional qualification, surgeon experience, case complexity stratification, and the management of key technical steps. Among these, appropriate selection of pancreaticojejunostomy plays a crucial role in reducing complications such as postoperative pancreatic fistula. From an oncologic perspective, MIPD can achieve margin status and R0 resection rates comparable to open surgery. Nevertheless, the persistently high rate of local recurrence and suboptimal long-term survival in pancreatic cancer indicate that true oncologic radicality remains unresolved. Traditional extended resections have not demonstrated clear survival benefits. Emerging concepts such as total mesopancreas excision offer new strategies for improving local control, but their anatomical basis, indications, and clinical value require further validation. With the increasing use of neoadjuvant therapy, inflammation and fibrosis further complicate anatomical identification, margin assessment, and intraoperative decision-making, thereby imposing higher demands on patient selection and surgical judgment. Overall, the evolution of MIPD should extend beyond technical minimal invasiveness toward a more balanced approach that integrates precise patient selection, rigorous difficulty stratification, and robust evidence-based support, aiming to achieve optimal oncologic outcomes without compromising safety.
-
ZHENG Shixu, TU Guangping, JIANG Haibo, XIE Shuangxi, LI Zhiqiang, YU Xiao
2026,35(3):446-457, DOI: 10.7659/j.issn.1005-6947.250702
Abstract:
Background and Aims Alcohol consumption is a major modifiable risk factor for pancreatitis. However, comprehensive evidence integrating the long-term disease burden of alcoholic pancreatitis and its causal relationship with acute and chronic pancreatitis remains limited. This study aimed to systematically evaluate the temporal trends, disease burden, and potential causal associations of alcoholic pancreatitis globally and in China using the Global Burden of Disease (GBD) 2021 database and two-sample Mendelian randomization (MR).Methods Data on deaths, disability-adjusted life years (DALYs), and corresponding age-standardized rates from 1990 to 2021 were extracted from the GBD 2021 database. Temporal trends were analyzed by sex and age group. Joinpoint regression was used to estimate the average annual percent change (AAPC), and decomposition analysis quantified the contributions of population growth, population aging, and epidemiological changes. A Bayesian age-period-cohort (BAPC) model was applied to project trends through 2040. Additionally, two-sample MR analysis based on publicly available GWAS summary statistics was conducted to assess the causal associations between alcohol consumption and pancreatitis.Results From 1990 to 2021, the numbers of deaths and DALYs attributable to alcoholic pancreatitis increased steadily both globally and in China, whereas age-standardized mortality and DALY rates declined or remained stable, with lower levels observed in China than the global average. The disease burden was substantially higher in males and older populations. Decomposition analysis indicated that population growth and aging were the primary drivers of the increased burden, while epidemiological changes contributed negatively. Projections suggested a continued slight decline in age-standardized burden, although the absolute burden will remain high. MR analysis demonstrated a robust positive causal association between genetically predicted alcohol consumption and increased risks of both acute and chronic pancreatitis.Conclusion Alcoholic pancreatitis exhibits a pattern of increasing absolute burden but declining age-standardized burden globally and in China, with marked age and sex disparities. Genetic evidence supports a positive causal relationship between alcohol consumption and pancreatitis risk. Strengthening alcohol control policies and targeted interventions is essential to reduce the long-term health and socioeconomic burden.
-
ZHAO Sicheng, LIU Baiqi, HUANG Gengwen
2026,35(3):458-469, DOI: 10.7659/j.issn.1005-6947.250538
Abstract:
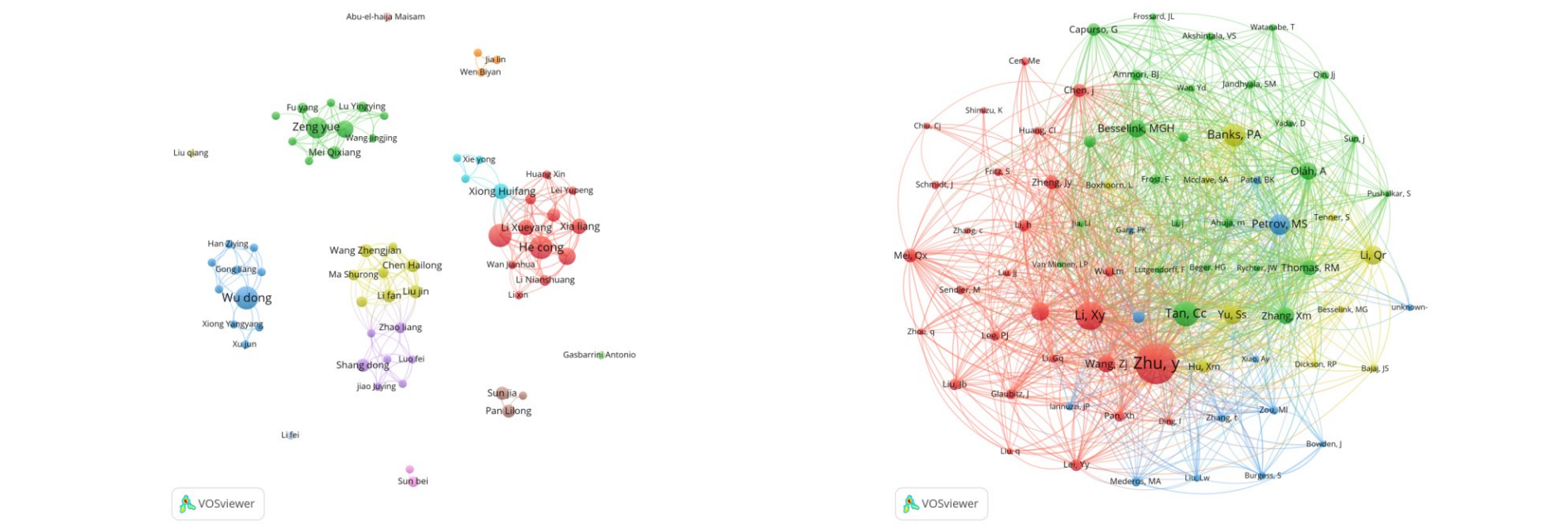
Background and Aims Acute pancreatitis (AP) is a heterogeneous disease with considerable mortality in severe cases. Increasing evidence highlights the critical role of the gut microbiome in AP progression; however, comprehensive bibliometric analyses in this field remain limited. This study aimed to systematically evaluate the research landscape and emerging trends of gut microbiome studies in AP.Methods Publications from January 2012 to February 2026 were retrieved from the Web of Science Core Collection. English articles and reviews related to AP and the gut microbiome were included. CiteSpace and VOSviewer were used to perform co-occurrence and clustering analyses of countries, institutions, authors, journals, and keywords. Publication trends were analyzed using GraphPad Prism.Results A total of 184 publications were included. The number of publications has increased steadily, with a rapid growth phase after 2019. China contributed the largest number of publications (n=141), and leading institutions were predominantly from China. Frontiers in Microbiology was the most productive journal, while Gut had the highest citation impact. Research hotspots mainly focused on gut microbiota dysbiosis and disease severity, intestinal barrier function, enteral nutrition, and microbiota-derived metabolites such as short-chain fatty acids and bile acids. Keyword clustering further highlighted complications of AP, intestinal barrier injury, and nutritional interventions as major research themes.Conclusion Research on the gut microbiome in AP is in a rapid development phase, with China playing a leading role. Future studies should focus on the interactions among gut microbiota dysbiosis, intestinal barrier dysfunction, and bacterial translocation, and integrate multi-omics and artificial intelligence approaches to advance precision medicine based on the gut-pancreas axis.
-
WANG Fengyi, SUI Yuhang, SUN Bei, LI Le
2026,35(3):470-479, DOI: 10.7659/j.issn.1005-6947.250643
Abstract:
Background and Aims Gut microbiota dysbiosis is implicated in the pathogenesis of chronic pancreatitis (CP), yet its causal relationship remains unclear. This study aimed to systematically evaluate the causal associations between gut microbiota and CP using Mendelian randomization (MR) integrated with multi-dimensional microbiome analyses.Methods Summary-level data from large-scale genome-wide association studies (GWAS) were used to perform two-sample MR analyses to assess the causal effects of gut microbial genera on CP and plasma metabolites. Fecal samples from CP patients and mouse models were subjected to 16S rRNA sequencing to characterize microbial alterations. Public datasets were incorporated for cross-validation to identify key CP-associated genera.Results MR analysis identified eight microbial genera with potential causal associations with CP. Lactococcus, Phascolarctobacterium, and Roseburia were identified as potential risk factors, whereas Methanobrevibacter and Lachnospiraceae FCS020 group showed protective effects. Additionally, 22 plasma metabolites were associated with CP. 16S rRNA sequencing revealed significant microbial dysbiosis, with 59 and 52 differentially abundant genera identified in humans and mice, respectively. Cross-validation consistently identified Lactococcus as the most critical genus across MR, human (P=0.008), and mouse (P=0.003) datasets.Conclusion By integrating genetic causal inference with microbiome profiling, this study provides evidence supporting a causal link between gut microbiota and CP. Lactococcus may exert stage-dependent effects, acting as a potential risk factor in disease susceptibility while being depleted during disease progression.
-
2026,35(3):480-487, DOI: 10.7659/j.issn.1005-6947.260122
Abstract:
Background and Aims Clinically relevant postoperative pancreatic fistula (CR-POPF) remains a major complication after pancreaticoduodenectomy (PD), significantly affecting patient outcomes. Conventional risk models have limitations in capturing complex nonlinear relationships. This study aimed to identify independent risk factors for CR-POPF and to develop and compare multiple machine learning-based prediction models.Methods A total of 334 patients who underwent PD at the Hepatobiliary and Pancreatic Center of Zhongda Hospital, Southeast University between January 2016 and December 2025 were retrospectively analyzed. Independent risk factors were identified using univariate and multivariate logistic regression analyses. The dataset was randomly divided into training and validation sets at a 7∶3 ratio. Prediction models were developed using Logistic regression (LR), artificial neural network (ANN), decision tree (DT), random forest (RF), and support vector machine (SVM). Model performance was evaluated using AUC, sensitivity, specificity, positive predictive value, negative predictive value, F1-score, and accuracy.Results Multivariate analysis identified increased BMI (OR=1.167), diabetes mellitus (OR=3.826), hypertension (OR=2.232), history of abdominal surgery (OR=2.599), lower preoperative albumin (OR=0.625), elevated postoperative white blood cell count (OR=1.091), and pancreatic-origin lesions (OR=2.945) as independent risk factors for CR-POPF (all P<0.05). Among the models, the ANN model demonstrated superior performance, with an AUC of 0.866, sensitivity of 0.745, specificity of 0.914, and F1-score of 0.768.Conclusion CR-POPF after PD is influenced by multiple clinical factors. The ANN-based model shows strong predictive performance and may serve as a valuable tool for early identification of high-risk patients and implementation of individualized interventions.
-
SUN Jing, LIU Yongrong, ZHANG Xin, CHANG Jingyu, ZHOU Nuying
2026,35(3):488-499, DOI: 10.7659/j.issn.1005-6947.250646
Abstract:
Background and Aims Pancreatic cancer has an extremely poor prognosis, and effective screening strategies for the general population are lacking. Circulating white blood cells are accessible immunoinflammatory markers, but their causal relationship with pancreatic cancer risk remains unclear. This study aimed to systematically evaluate the potential causal associations between peripheral white blood cell counts and pancreatic cancer risk using Mendelian randomization (MR).Methods A two-sample MR design was applied. GWAS summary statistics for total white blood cell count and five major subtypes were obtained from the Blood Cell Consortium. Pancreatic cancer outcome data were derived from FinnGen release 12 (European population), with additional validation using East Asian GWAS datasets. The inverse-variance weighted (IVW) method was used as the primary analysis, complemented by multivariable MR, reverse MR, and multiple sensitivity analyses.Results Univariable MR analysis showed that genetically predicted higher eosinophil count was associated with a lower risk of pancreatic cancer (IVW: OR=0.886, 95% CI=0.793-0.990, P=0.033), with consistent direction across methods. Multivariable MR confirmed that this protective association persisted after adjusting for other leukocyte subtypes (OR=0.848, 95% CI=0.723-0.995, P=0.043). Reverse MR provided no evidence for a causal effect of pancreatic cancer on white blood cell traits. The East Asian validation analysis showed a consistent direction of effect. No robust associations were observed for other leukocyte traits.Conclusion Genetically predicted higher eosinophil levels may be associated with a reduced risk of pancreatic cancer. These findings provide supportive evidence for the immunoetiology of pancreatic cancer, but are not yet sufficient for direct clinical application.
-
WANG Dali, FEI Haoran, SUN Dan, YANG Haishen, HU Wei
2026,35(3):500-511, DOI: 10.7659/j.issn.1005-6947.250647
Abstract:
Background and Aims Proteasome 20S subunit β2 (PSMB2) has been implicated in tumor progression in multiple cancers; however, its expression pattern, prognostic value, and underlying mechanisms in pancreatic ductal adenocarcinoma (PDAC) remain unclear. This study aimed to investigate the clinical significance and potential mechanisms of PSMB2 in PDAC through integrated bioinformatics analysis and clinical validation.Methods Expression profiles and clinical data from TCGA and GEO datasets (GSE62452 and GSE15471) were analyzed to evaluate PSMB2 expression and its prognostic significance. Kaplan-Meier survival analysis and Cox regression models were used. Immunohistochemistry was performed on 76 PDAC samples for validation. Gene Set Enrichment Analysis (GSEA) and correlation analyses were conducted to explore potential mechanisms. Immune cell infiltration was assessed using ssGSEA, and immunotherapy response was predicted using TCIA data. Drug sensitivity was analyzed based on the GDSC database.Results IPSMB2 expression was significantly upregulated in PDAC tissues, and high expression was associated with poorer overall survival (all P<0.05). Multivariate Cox analysis identified PSMB2 as an independent prognostic factor. Immunohistochemical results were consistent with bioinformatics findings. PSMB2 expression correlated with lymph node metastasis, pathological stage, and differentiation. GSEA indicated enrichment in the ECM-receptor interaction pathway. Correlation analysis showed positive associations with multiple ECM-related genes. Additionally, PSMB2 was associated with immune cell infiltration and predicted immunotherapy response. Higher PSMB2 expression was also linked to increased sensitivity to several targeted agents.Conclusion PSMB2 is overexpressed in PDAC and is associated with poor prognosis, serving as an independent prognostic biomarker. Its role may involve regulation of the ECM-receptor interaction pathway and tumor immune microenvironment, highlighting its potential as a therapeutic target.
-
TU Guangping, CHEN Lang, HUANG Hui, YU Xiao, LI Zhiqiang, YU Can, LIU Yunfei
2026,35(3):512-523, DOI: 10.7659/j.issn.1005-6947.250396
Abstract:
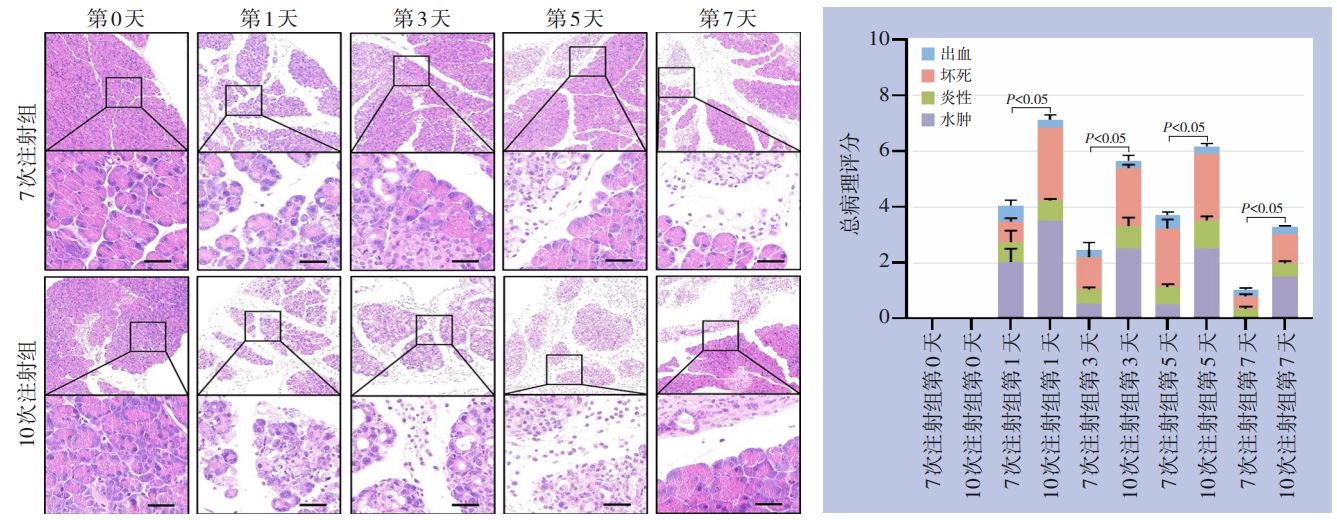
Background and Aims Pancreatic regeneration following acute pancreatitis (AP) exhibits marked heterogeneity, which is closely related to the initial injury severity but remains insufficiently characterized. This study aimed to investigate the pathological features of pancreatic regeneration and repair under different injury severities.Methods Cerulein-induced AP mouse models were established using two regimens: 7 injections (mild injury) and 10 injections (moderate-to-severe injury). Pancreatic tissues were collected on days 1, 3, 5, and 7. Histopathological injury was evaluated using HE staining and scoring. Immunofluorescence was used to assess acinar-to-ductal metaplasia (ADM) markers (CK19, SOX9) and macrophage polarization markers (F4/80, iNOS, CD206). Fibrosis was evaluated by Masson staining and α-SMA immunohistochemistry. Cell proliferation was assessed by Ki-67 staining.Results The 10-injection group exhibited significantly more severe pancreatic injury and delayed repair compared with the 7-injection group (P<0.05). ADM was markedly enhanced, with increased expression of CK19 and SOX9. Macrophage infiltration was elevated with a predominance of M1 polarization. Fibrosis was significantly aggravated, as evidenced by increased collagen deposition and α-SMA expression (P<0.05). Cell proliferation showed a pattern of early activation with a delayed peak. In contrast, the 7-injection group showed localized injury and rapid recovery with milder pathological changes.Conclusion Different cerulein injection regimens induce graded injury phenotypes in AP mice. Pancreatic regeneration exhibits injury severity-dependent heterogeneity, involving coordinated regulation of ADM, macrophage polarization, fibrosis, and cell proliferation.
-
LI Ziyi, GUO Siqi, XIE Peiqin, ZHANG Min, ZHONG Xiaohua, WEI Xiuwen, HU Chen
2026,35(3):524-534, DOI: 10.7659/j.issn.1005-6947.250370
Abstract:
Background and Aims Pancreatic cancer is highly malignant with poor prognosis, and effective molecular targets are still lacking. Actin filament-associated protein 1-like 2 (AFAP1L2) has been reported to promote tumor progression in multiple cancers; however, its role in pancreatic cancer remains unclear. This study aimed to investigate the expression profile and functional mechanism of AFAP1L2 in pancreatic cancer.Methods Bioinformatics analysis and Western blot were used to evaluate AFAP1L2 expression in pancreatic cancer tissues and cells, and its association with patient survival was analyzed. AFAP1L2 was silenced by shRNA, and cell proliferation, invasion, and migration were assessed using CCK-8, colony formation, Transwell, and wound healing assays. EMT markers and RAS/ERK pathway-related proteins were detected by Western blot. A nude mouse xenograft model was established to validate in vivo effects. RAS-GTP levels and co-immunoprecipitation assays were performed to explore the underlying mechanism.Results AFAP1L2 was highly expressed in pancreatic cancer tissues and cells and was negatively correlated with patient survival. Silencing AFAP1L2 significantly inhibited cell proliferation, invasion, and migration in vitro and suppressed tumor growth in vivo. Mechanistically, AFAP1L2 interacted with RASA1 and inhibited its GTPase-activating activity, leading to increased RAS-GTP levels and activation of the RAS/ERK pathway. Knockdown of AFAP1L2 restored RASA1-mediated negative regulation of RAS, decreased ERK and MEK phosphorylation, and attenuated malignant progression.Conclusion AFAP1L2 promotes proliferation and metastasis of pancreatic cancer cells by activating the RAS/ERK signaling pathway through inhibition of RASA1, suggesting its potential as a therapeutic target.
-
LIU Xing, ZHOU Zhengtao, WU Xiaoping, LIU Jie, YANG Xuli
2026,35(3):535-542, DOI: 10.7659/j.issn.1005-6947.240677
Abstract:
Background and Aims Hepatocellular carcinoma (HCC) with portal vein tumor thrombus (PVTT) is associated with extremely poor prognosis. Identification of prognostic factors is essential for clinical decision-making. This study aimed to investigate survival-related prognostic factors in HCC patients with PVTT based on real-world data.Methods A total of 195 patients with HCC and PVTT admitted to the First Affiliated Hospital of Nanchang University between January 2019 and December 2021 were retrospectively enrolled and followed up until December 2022. Survival analysis was performed using the Kaplan-Meier method. Univariate analysis was conducted using the Log-rank test, and multivariate analysis was performed using the Cox proportional hazards model.Results During follow-up, 162 patients (83.08%) died. The median survival time was 114 (102-126) d. The 30-, 90-, 180-d, and 1-, 2-, and 3-year survival rates were 82.56%, 56.41%, 38.97%, 26.67%, 18.46%, and 16.92%, respectively. Univariate analysis identified age, performance status (PS), albumin, total bilirubin (TBIL), and lymphocyte count as significant prognostic factors (all P<0.05). Multivariate analysis revealed that PS>2, lymphocyte count <1.7×109/L, and TBIL>26 μmol/L were independent predictors of poor prognosis (all P<0.05).Conclusion Patients with HCC and PVTT have poor overall survival. Elevated PS score, lymphopenia, and increased bilirubin levels are independent adverse prognostic factors, which may serve as useful indicators for risk stratification and individualized treatment.
-
YU Xiaofeng, HE Qian, CHEN Peng, WANG Xiaoli, LIU Xin
2026,35(3):543-549, DOI: 10.7659/j.issn.1005-6947.250136
Abstract:
Background and Aims Postoperative lymph node metastasis is a major determinant of prognosis in colorectal cancer (CRC). However, reliable and convenient preoperative predictive tools remain limited. Inflammatory markers derived from routine blood tests, such as neutrophil-to-lymphocyte ratio (NLR) and platelet-to-lymphocyte ratio (PLR), have shown potential prognostic value. This study aimed to identify risk factors and develop a predictive model for postoperative lymph node metastasis in CRC patients.Methods A total of 125 CRC patients who underwent radical surgery between January 2020 and December 2023 were retrospectively enrolled and followed for one year. Patients were divided into metastasis (n=31) and non-metastasis groups (n=94). Clinicopathologic features and preoperative blood parameters were collected. Univariate analysis and multivariate logistic regression were performed to identify independent risk factors. A nomogram model was constructed and evaluated using the concordance index (C-index), calibration curve, and receiver operating characteristic (ROC) curve.Results Univariate analysis showed that tumor size ≥3 cm, poor differentiation, submucosal invasion, vascular invasion, elevated neutrophil count, monocyte count, platelet count, PLR, NLR, and decreased lymphocyte count were significantly associated with lymph node metastasis (all P<0.05). Multivariate analysis identified poor differentiation (OR=2.044), submucosal invasion (OR=2.643), vascular invasion (OR=2.542), high PLR (OR=3.022), and high NLR (OR=2.380) as independent risk factors (all P<0.05). The nomogram achieved a C-index of 0.881 (95% CI=0.828-0.934), with good calibration. The AUC was 0.874 (95% CI=0.821-0.927), with a sensitivity of 91.66% and specificity of 68.05%.Conclusion The nomogram integrating pathological features and blood-derived inflammatory markers demonstrates good predictive performance for postoperative lymph node metastasis in CRC patients and may assist in individualized clinical decision-making.
-
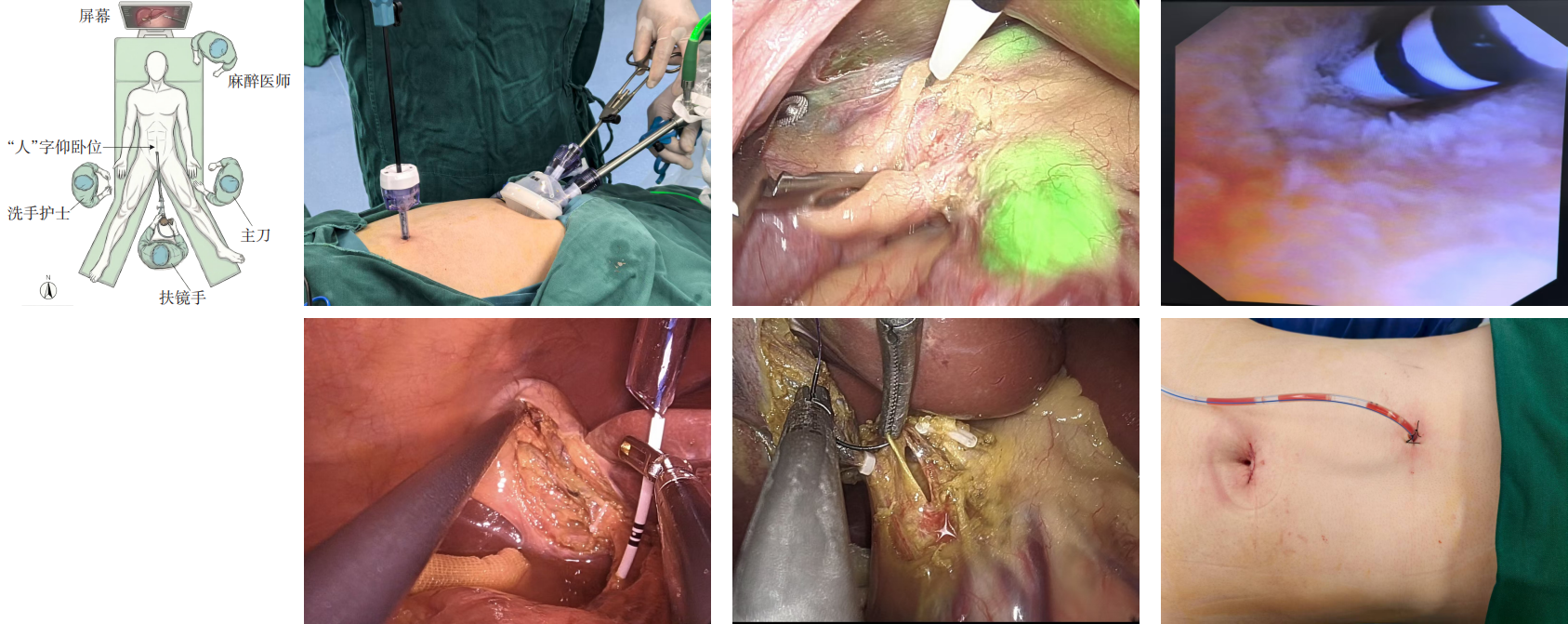
XIANG Guangming, ZHANG Jixiong, YANG Maozhu, YANG Ke, YAN Su, DONG Jiangkun, LAI Chunyou, WANG Guan, TANG Hong, ZHOU Guo, YAO Yutong
2026,35(3):550-557, DOI: 10.7659/j.issn.1005-6947.250544
Abstract:
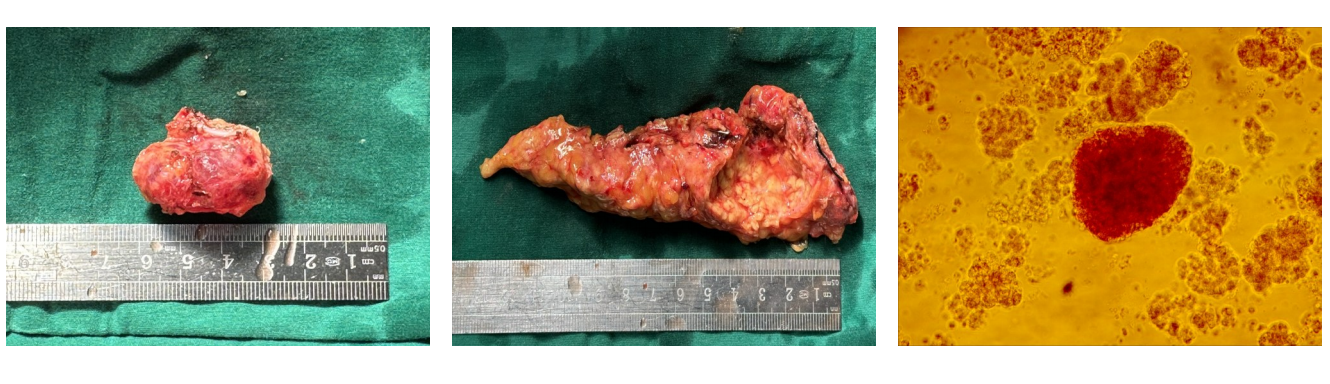
Background and Aims Laparoscopic spleen-preserving distal pancreatectomy (LSPDP) is a standard procedure for intraductal papillary mucinous neoplasms (IPMN) of the pancreatic body and tail, but it may increase the risk of postoperative type 3c diabetes mellitus (T3cDM) due to loss of normal pancreatic tissue. Autologous islet transplantation (AIT) may preserve endocrine function; however, its application in IPMN remains controversial. This study aimed to evaluate the safety and feasibility of LSPDP combined with AIT.Methods A 56-year-old woman with IPMN underwent LSPDP combined with AIT. A total of 41.6 g of pancreatic tissue was resected, and islets were isolated in a GMP facility, yielding 1 139 IEQ/kg with 20% purity and 97% viability. Islets were infused into the portal vein under laparoscopic and intraoperative ultrasound guidance. Postoperative management included anticoagulation, nutritional support, and strict glycemic control.Results The postoperative course was uneventful, with no complications such as bleeding, infection, portal vein thrombosis, pancreatic fistula, or tumor recurrence. During 1-year follow-up, fasting and postprandial glucose levels and C-peptide remained within normal ranges, and no T3cDM occurred. Imaging showed no evidence of recurrence, and endocrine function was well preserved.Conclusion Under strict patient selection and oncological safety, LSPDP combined with AIT may achieve tumor resection while preserving endocrine function in IPMN patients, demonstrating favorable short-term safety and feasibility. Long-term metabolic and oncological outcomes require further validation.
-
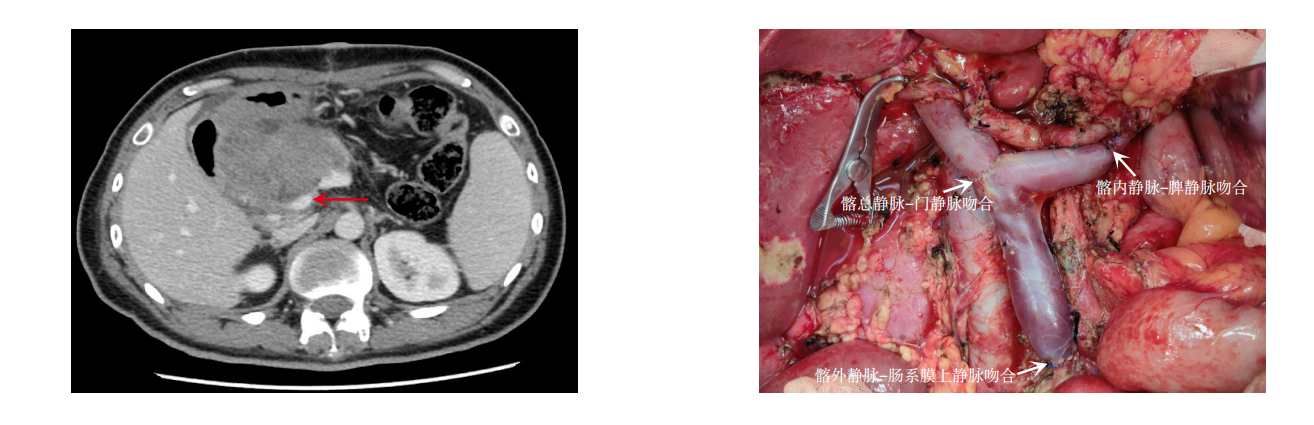
GUO Yu, LEI Lei, JIN Kui, NIU Quan, ZHANG Tao, JI Wangming, ZHAO Di, YAN Tao, LU Wei, DUAN Weihong, LIU Jungui
2026,35(3):558-564, DOI: 10.7659/j.issn.1005-6947.260129
Abstract:
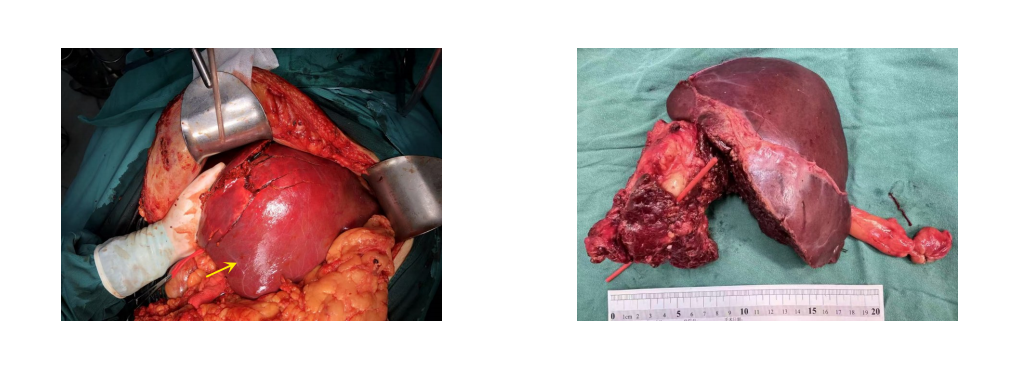
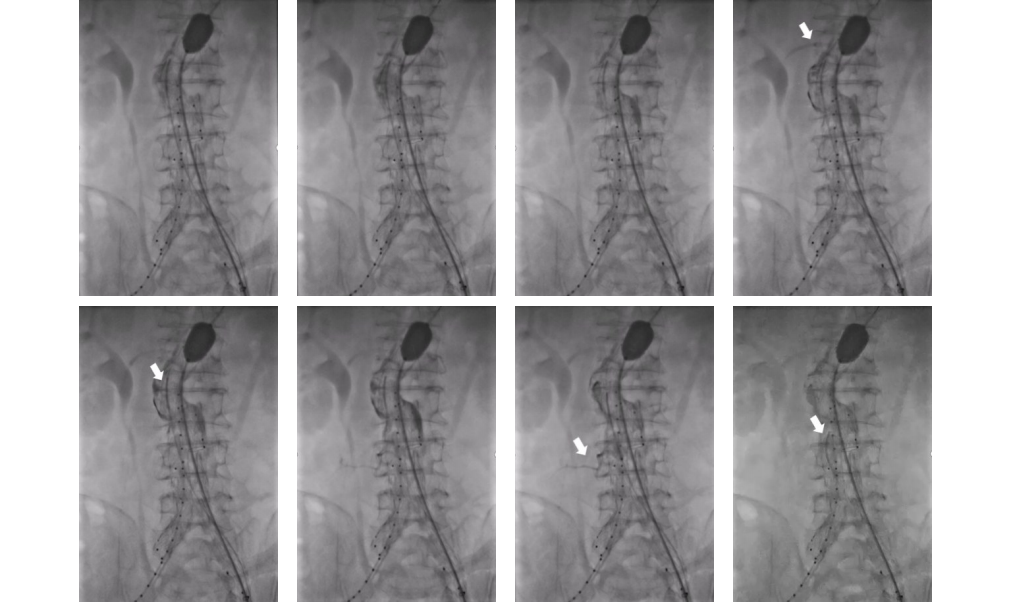
Background and Aims When pancreatic tumors invade the portal vein-superior mesenteric vein, especially with involvement exceeding 5 cm, end-to-end anastomosis is often not feasible, limiting the achievement of R0 resection. This study aimed to evaluate the feasibility and safety of using allogeneic common iliac vein and its branches for Y-shaped vascular reconstruction.Methods A retrospective analysis was conducted on two patients with pancreatic tumors involving long-segment portal vein-superior mesenteric vein treated between May 2022 and April 2024. Both patients underwent en bloc tumor and venous resection. Allogeneic common iliac vein with its branches was trimmed into a Y-shaped graft to reconstruct the portal vein-superior mesenteric vein and portal vein-splenic vein pathways.Results Both surgeries were successfully completed without major perioperative complications or venous thrombosis. The postoperative hospital stays were 27 and 23 days, respectively. Pathology revealed a solid pseudopapillary tumor in case 1 and poorly differentiated pancreatic adenocarcinoma in case 2. Case 1 remained recurrence-free at 12-month follow-up, whereas case 2 developed liver metastasis and died 4 months postoperatively. Postoperative imaging demonstrated good graft patency and effective restoration of splanchnic venous return.Conclusion For pancreatic tumors with portal vein-superior mesenteric vein involvement exceeding 5 cm, Y-shaped reconstruction using allogeneic common iliac vein and its branches is feasible and safe in the short term, enabling R0 resection while restoring both mesenteric and splenic venous return. Larger studies are needed for further validation.
-
BIAN Jie, MENG Xingkai, ZHANG Ming, GUO Yan, LIU Na, LI Jun
2026,35(3):565-572, DOI: 10.7659/j.issn.1005-6947.260021
Abstract:
Postoperative pancreatic fistula (POPF) remains a major complication affecting prognosis after pancreaticoduodenectomy (PD), closely associated with the healing of pancreaticojejunostomy. This review systematically summarizes recent advances in the key factors influencing anastomotic healing after PD from three aspects: preoperative assessment, intraoperative techniques, and postoperative management. Preoperatively, soft pancreatic texture, small main pancreatic duct, obesity, and inflammatory-nutritional markers (such as the C-reactive protein-to-albumin ratio) are identified as major risk factors. Intraoperatively, the choice of anastomotic technique should be individualized based on pancreatic characteristics, while novel suture materials, robotic assistance, and emerging biomaterials (e.g., hydrogels) show promising potential in reducing POPF risk. Postoperatively, control of bacterial colonization in drainage fluid, early drain removal, and strict glycemic management play critical roles in anastomotic healing. Future studies should focus on elucidating multifactorial synergistic mechanisms, developing dynamic predictive models, and validating new techniques and biomaterials through high-quality clinical trials to achieve precision and individualized management of POPF.
-
SONG Xingchao, MA Xiao, HE Zifan, YANG Weibin, XU Anzhi, TIAN Chunyan
2026,35(3):573-578, DOI: 10.7659/j.issn.1005-6947.260081
Abstract:
T-cell lymphoma invasion and metastasis-inducing factor 1 (TIAM1) is a guanine nucleotide exchange factor (GEF) that plays a crucial role in tumorigenesis and progression. Increasing evidence has demonstrated that TIAM1 is highly expressed in pancreatic cancer and is closely associated with tumor proliferation, invasion, metastasis, and poor prognosis. This review summarizes the current advances in understanding the biological functions and molecular mechanisms of TIAM1 in pancreatic cancer. Particular emphasis is placed on the TIAM1-Rac1 signaling axis and its crosstalk with Wnt/β-catenin and RhoA pathways, as well as its roles in cytoskeletal remodeling, epithelial–mesenchymal transition (EMT), and metabolic reprogramming. In addition, the potential involvement of TIAM1 in shaping the tumor immune microenvironment is discussed. TIAM1 may serve as a promising prognostic biomarker and therapeutic target, and further elucidation of its regulatory network could provide novel insights for precision therapy in pancreatic cancer.
-
HU Zongyi, WANG Zihan, XING Jiayi, ZHANG Yueqing, WANG Wenwen, WANG Tianze, LI Cheng, ZHANG Wei
2026,35(3):579-587, DOI: 10.7659/j.issn.1005-6947.250286
Abstract:
Pancreatic cancer is a highly aggressive malignancy with an extremely poor prognosis, in which the immunosuppressive tumor microenvironment plays a pivotal role in disease progression. Interleukin-1β (IL-1β), a key pro-inflammatory cytokine, is critically involved in inflammation, fibrosis, epithelial-mesenchymal transition (EMT), and immune regulation. Accumulating evidence indicates that IL-1β contributes to the initiation, progression, and metastasis of pancreatic cancer through multiple signaling pathways, and is closely associated with poor prognosis, therapeutic resistance, and tumor recurrence. Notably, IL-1β may also exert anti-tumor effects under specific conditions, highlighting its context-dependent dual role. This review systematically summarizes the biological characteristics of IL-1β and its multifaceted roles in the pancreatic tumor microenvironment, with a focus on its potential applications in diagnosis, prognostic evaluation, and targeted therapy. Current controversies and future research directions are also discussed.
Volume 35,2026 Number 3
GUIDELINE AND CONSENSUS
COMMENTARY
SPECIALIST FORUM
MONOGRAPHIC STUDY
BASIC RESEARCH
CLINICAL RESEARCH
TECHNIQUE IMPROVEMENT
REVIEW
-
Department of Medical Administration, National Health Commission of the People''s Republic of China
Abstract:
In April 2024, the "Guidelines for the diagnosis and treatment of primary liver cancer (2024 edition)"were officially released. The guidelines were developed by experts and scholars from various disciplinesin the field of liver cancer across the country under the leadership of the Department of MedicalAdministration of the National Health Commission of the People""s Republic of China and with guidancefrom the Expert Committee on the Compilation of Guidelines for the Diagnosis and Treatment ofPrimary Liver Cancer, the National Cancer Center, and the Liver Cancer QualityControl ExpertCommittee of the National Cancer Quality Control Center. The main updates in the "Guidelines for thediagnosis and treatment of primary liver cancer (2024 edition)" include: updates tosurgical treatmentmethods and concepts; objective evaluation of the value of local ablation; revitalization of vascular ntervention therapy; further exploration and optimization of radiotherapy; and significant breakthroughsin systemic treatment. As a normative guidance document for primary liver cancer, the guidelines keeppace with the times, timely reflecting new developments and concepts in the field of liver cancerdiagnosis and treatment, which will effectively drive the elevation of standardized diagnosis and treatment levels for liver cancer in China, enhanced the influence of our country in this field within the academic community, and hold high guiding significance for the future